share
Anxiety

Conventional Treatment Options
There are many forms of anxiety including post-traumatic stress disorder (PTSD), obsessive-compulsive disorder (OCD), panic disorder, phobias, social anxiety disorder (SAD), agoraphobia, and generalized anxiety disorder (GAD).
In the U.S., psychological approaches and antidepressants are "first line" treatments. In the U.K., guidelines are more cautious with drugs, only nondrug treatments are recommended as first-line treatments. [1]
These guidelines underscore that drugs are far from a complete solution. To maximize recovery, anxiety is best viewed in a broader context that considers drugs' partial effectiveness, risks, and limitations as well as the many evidence-based nondrug options available (see free monograph). This full view helps individuals and their practitioners make the most informed choices about care.
Antidepressants: benefits, risks, & limitations
A sobering review of gold standard evidence
Benefits. Although antidepressants can help some, overall they work only modestly better than sugar pills for anxiety: 50% of people respond to placebo while 68% respond to antidepressants. [2] In fact, only 1 in 5 people with generalized anxiety and PTSD see substantial benefit attributable to antidepressants. [3] One large analysis found that this benefit has even been overestimated, and in some cases is no better than placebo. [4] .For OCD psychological approaches are clearly better than antidepressants. [5}
Side effects. 86% of people have side effects and 55% find them bothersome. [6] These include weight gain, gastrointestinal issues, cardiovascular issues, and Parkinsons-like involuntary movements. [7] They can persist even after you stop using antidepressants. The FDA warns that SSRI antidepressants double the frequency of suicidal thoughts in those under 25. [8] Use also triples the frequency of aggressive behavior in children.[9]
Elevated long-term risk. Although there is little research on the long-term use of antidepressants for anxiety, the results for depression are grim. Depressed people on antidepressants show significantly worse depression at 9-year, 20-year, and 30-year follow-up visits as compared to depressed individuals who did not take these drugs. [10]
Withdrawal difficulty. Noted psychiatrist Dr. Allen Francis warns of Antidepressant Discontinuation Syndrome "It’s so easy to start an antidepressant and sometimes so very difficult to stop." [11] 56% of people experience withdrawal, 46% of these find it severe. [12] Withdrawal symptoms include dizziness, anxiety, irritability, poor concentration, gastrointestinal problems, and more. [13] The duration of withdrawal difficulty averages 50 weeks for those on SNRI antidepressants, and 90 weeks for those on SSRIs. [14]
Post SSRI Sexual Dysfunction (PSSD). Evidence suggests that the sexual dysfunction common in SSRI antidepressant use may persist even after the drugs are discontinued. Common PSSD symptoms include genital anesthesia and pleasure-less or weak orgasm. There is currently no treatment for PSSD. [15]
Blunting of Empathy. Antidepressants can limit the ability to feel normal emotions. One study found that after using them for three months, people have less ability to empathize with others and scans indicate reduced activity in portions of the brain associated with empathy. [16]
Esketamine: even greater risk. The new antidepressant Esketamine comes with even greater risks than older antidepressants. FDA warnings highlights the potential for sedation, dissociation, attention and judgment problems, drug abuse, suicidal thoughts, and suicidal behavior. As a result, the FDA has placed restricted availability and tight monitoring on the drug. [17]
Faulty grounding theory. A fundamental reason for the poor outcomes with antidepressants is that experts now consider the underlying chemical imbalance theory to be a "gross over-simplification". [18] A one-size-fits-all drug approach doesn't match the complex human experience of mental distress. Many psychiatrists and researchers agree that a more sophisticated theory and therapeutic approach is needed. Dr. Joanna Moncrieff explains in this video.
Benzodiazepines: benefits, risks, & limitations
A sobering review of gold standard evidence
Benefits. Benzodiazepines (benzos) are well tested and can often provide fairly immediate and effective relief from anxiety symptoms. They are used as a sedative and anesthetic, and can promote a sense of calm. However, they are for limited use and come with many troubling issues (see graphic).
Long-term risk. Prescribing guidelines are limited to 1-28 days [19] due to serious issues with prolonged use. These include greater risk of anxiety, mood episodes, amnesia, cognitive decline, and suicide. Because they sedate, they are associated with increased hip fractures from falls, industrial accidents, and car accidents. [20] In addition, the FDA has issued their most severe alert - a black box warning - because benzos can cause death if taken with opioids. [21]
Dependence and addiction. Benzos are a DEA controlled substance due to their addictive potential. Withdrawal can be very difficult and sometimes lasts months or years. The FDA gives benzos its most severe warning label because of the sizable risks of abuse, misuse, addiction, physical dependence and withdrawal reactions. [22] American Addiction Centers emphasizes that they can cause both physical and psychological dependence. [23] The high prescribing rates - tripling over an 18 year period - and the drug's addictive nature has contributed to a sharp increase in benzo overdose deaths that researchers warn may be a potential epidemic akin to opioids. [24]
Controversy. There remains a significant controversy about whether the short-term benefits of benzos outweigh the risk of dependence. [25] This is especially true for the elderly since they are at the greatest risk of experiencing side effects. Despite warnings, benzo prescribing remains common for the elderly, and women are twice as likely as men to be given prescriptions. [26]
Psychosocial Therapies
Evidence from gold-standard studies
There are many psychosocial therapies for the various forms of anxiety (see diagram). Studies show them as effective or better than drugs, rarely with side effects, and unlike drugs, they offer long-term benefit after use.
Cognitive Behavioral Therapy (CBT). CBT helps us replace unhelpful thoughts with more constructive ones which helps us better direct our emotions, and actions. CBT is effective for nearly every diagnosis.
Mindfulness. Mindfulness is being calm, relaxed, and focused. It is one of the most proven techniques for improving mental well-being. It includes a variety of techniques that help us become alert, aware, and peaceful. It is formalized into a wellness program (Mindfulness-Based Stress Reduction) and included in CBT (Mindfulness-Based Cognitive Therapy).
Exposure Therapy. Exposure therapies help resolve past trauma and obsessive thoughts by going to the heart of it: slowly re-experiencing it in our mind so that we can loosen its grip and choose a better response.
Eye Movement Desensitization & Reprocessing (EMDR) and Emotional Freedom Technique (EFT). Two trauma processing techniques that use physical acts (eye movement vs. acupoint "tapping") that don't require the degree of direct re-experiencing of trauma found in Exposure Therapy.
Psychodynamic Psychotherapy. One-on-one therapist dialogue probing unconscious influences of our emotions, thinking, and behavior.
And more. Other approaches include Psychoeducation, Peer Support, Interpersonal Psychoterhapy, Behavioral Activation, Motivational Interviewing, Somatic Experiencing, Biofeedback, support groups, and MDMA-assisted psychotherapy. Often the quality of relationship with the therapist is as important as the specific therapy.
Delivery methods. All of these therapies can be delivered by a therapist. Many online, app, and self-help versions exist as well.
A New Paradigm: Integrative Mental Health
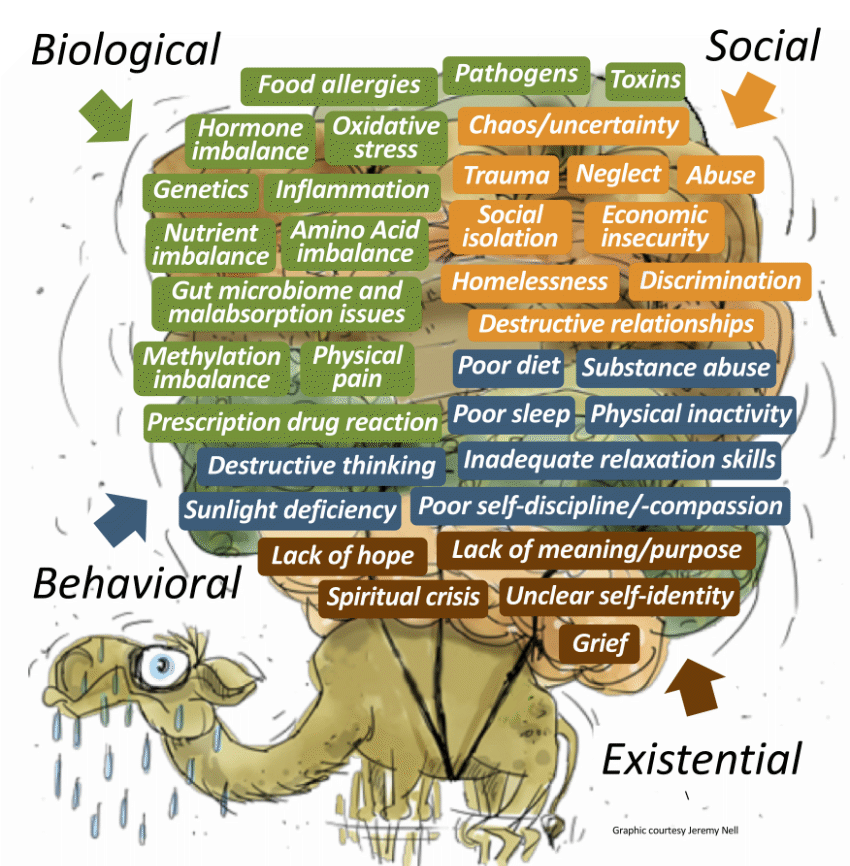
Looking beyond symptoms to causes. Many practitioners are adopting an extended paradigm that looks beyond drugs. They see numerous factors dynamically interacting to cause mental distress - many we understand, others we don't. The combined weight of these factors can lead to episodes of anxiety and sometimes "break the camel's back" and precipitate crisis (see graphic).
Offering personalized care. Integrative practitioners delve deeply into the unique constellation of causative factors facing each individual using detailed diagnostic tools. From this analysis they create personalized treatment plans.
Using a broad menu of options. Integrative Mental Health treatment plans nearly always include targeted evidence-based nondrug options. These options are drawn from 27 broad nondrug approaches shown effective for mental wellness. Nearly all options can be used with drugs, they typically have far fewer and milder side effects than drugs, and in many cases their use can reduce - and in some cases eliminate - the need for drugs.
Delivering better outcomes. Drugs alone rarely deliver recovery. Thankfully, you have options. There are hundreds of gold-standard studies that show anxiety relief from nondrug options. [27] Limiting yourself to drugs limits your avenues to wellness and avoids the symptom relief available in nondrug options.
Providing options people prefer. A review of 34 studies found that people prefer psychological treatments over drugs 3 to 1. [28]
Defining a new discipline. Many psychiatrists, GPs, nurse practitioners, naturopaths, therapists, medical specialists, and others are joining the paradigm shift to Integrative Mental Health, a discipline that spans the best of drug and non-drug care. These practitioners see that our mind, body, and emotions require a more holistic solution than pills alone can provide. They acknowledge a role for drugs, but consider them with great caution, especially for the developing brain and personhood of children.

Wellness Continuum
4 forms of care for
anxiety

Adapted from the U.S. Institute of Medicine and European Union of General Practitioners/Family Physicians. [35]
Back to Basics
Preventive
Preventive approaches help us avoid anxiety. These include proper diet, aerobic exercise, mindfulness, stress management, ensuring gut-health, social interaction, mind-body disciplines (especially yoga) and more.
Restorative
Two methods work to address causative factors of anxiety.
Biomedical practitioners (see practitioner finder) help identify and support your unique bio-individuality using robust lab tests. Testing helps uncover nutrient imbalances, hormonal issues, amino acid irregularities, food allergies, inflammation, and other issues that are directly associated with anxiety.
Psychosocial practitioners help address painful human experiences including trauma, dysfunctional relationships, unhelpful thinking, and more. The psychosocial therapies outlined above target these causative factors. Often the quality of the patient-therapist relationship is as important as the type of psychosocial therapy used. Spiritually-sensitive care can help those experiencing difficult personal growth.
Symptom Relief
Symptom relief addresses residual symptoms not removed by preventive and restorative care. Various herbs, nutrients, sensory therapies, and more have been shown effective.
Over-care
Avoidance
Over-care avoidance limits interventions (often drugs) to only what is necessary.
Too much care can be expensive and harmful.
This is especially true with benzodiazepines. Their overuse can lead to addiction and significant cognitive decline and increased suicidality.
It is often best to avoid drugs as a first line treatment since they do not cure and typically do not work as well as appropriate psychosocial therapies.
Many psychiatrists are considering de-prescribing plans with their patients based on tantidepressant's and benzodiazepine's risk/benefit profile. [29]
Your life. Your choice.
The limited effectiveness and many challenges of antidepressants and benzodiazepines make their risk/reward profile much less favorable than most people think.
This is one reason why key voices in mainstream psychiatry support nondrug options.
-
NAMI. Dr. Kenneth Duckworth, Medical Director of the National Alliance on Mental Illness, is clear: "... psychiatric medications... are rarely enough to promote recovery alone... Use of non-medication strategies is crucial for most clinical situations." [30]
-
Mental Health America advocates many nondrug options. [31]
-
American Psychiatric Association sponsors a special interest caucus of psychiatrists grounded in Integrative Mental Health. [32]
In addition, Dr. James Scully, past American Psychiatric Association Medical Director and CEO, understands well the implications of psychiatric drugs. He says:
Physicians and patients together should be thinking carefully, ‘Are the medications really needed and are there downsides and negative consequences for overuse?’... Patients really need to be a part of the decision… of their own treatments. [33]
Carefully consider Dr. Scully’s question – your recovery may well depend on it – and be an active participant in determining your treatment. If you make adjustments to the drugs you take, do so slowly under practitioner care.
Unfortunately, communication about nondrug options rarely occurs. [34]
Always work closely with your doctors as you make care decisions. They are your trusted guides. Also independently educate yourself since Integrative Mental Health is not yet prevalent in psychiatric care. You will likely need to expand your team to include integrative practitioners if you seek to use nondrug options as part of your recovery.
Although non-drug options aren't a panacea, many people are reclaiming their lives thanks to the expanded menu of options of Integrative Mental Health. Their self-determined return to normalcy can offer you compelling and pragmatic reasons for hope.



Resources
-
Free! Anxiety Monograph - Overview of non-drug options
-
Choices in Recovery - Detail on evidence-based non-drug options for anxiety and other major diagnoses.
-
Effective psychosocial Therapies for anxiety as compiled by the Psychological Associations of Australia, Canada, the U.K. and the U.S.
Footnote references are removed in the mobile version of this page to respect small screen sizes.
They can be found in the desktop version.
share
Note: To make this material more understandable, we use commonly understood phrases to represent rigorous statistical metrics. See our definitions.
References:
[1] National Institute for Health Care Excellence, Anxiety Disorders, 2014, copied Nov 2018 from https://goo.gl/7qhXE5, https://goo.gl/5TLhsD.
[2] Baldwin D et al, Evidence-based pharmacological treatment of generalized anxiety disorder, Int J Neuropsychopharmacology, 2011, PMID: 21211105, https://goo.gl/v5a3QF. Note: "...approximately 40–60% of patients ‘respond’ to placebo and 60–75% to the selective serotonin reuptake inhibitor (SSRI) compounds..." 40-60% averages to 50%, 60-75% verages to 68%.
[3] Note:"benefit attributable to" teases apart the true value of a treatment from its placebo effect and refers directly to "Number Needed to Treat" (NNT), recognized as the best way to evaluate treatment efficacy. The word "substantial" is used as a proxy for "response" to highlight that there is an improvement threshold ("response") implicit in NNT. Using "substantial medicinal value" helps avoid a statistical discussion of NNT which is beyond the scope of interest for the intended audience, but such discussion is available here as needed. The NNT for antidepressants for GAD is somewhat greater than 5, so 1 in 5 see "substantial medicinal value" with antidepressants, while 4 in 5 do not. Flynn C et al, Antidepressants for Generalized Anxiety Disorder, American Family Physician, 2003, https://goo.gl/2AH9Cq, "...The calculated NNT for antidepressants in GAD is 5.5... Schmitt R et al, The efficacy of antidepressants for generalized anxiety disorder: a systematic review and meta-analysis, Braz J Psychiatr. 2005, PMID: 15867979. "...The calculated number needed to treat for antidepressants in generalized anxiety disorder was 5.15"... Stein DJ, Pharmacotherapy for post traumatic stress disorder (PTSD), Cochrane Database Syst Rev. 2006, PMID: 16437445. '..overall superiority of a variety of medication agents to placebo (relative risk 1.49, 95% CI 1.28 to 1.73, number needed to treat = 4.85, ..." . See www.TheNNT.com for a detailed discussion on NNT.
[4] Roest AM, Reporting Bias in Clinical Trials Investigating the Efficacy of Second-Generation Antidepressants in the Treatment of Anxiety Disorders: A Report of 2 Meta-analyses, JAMA Psychiatry. 2015, PMID: 25806940
[5] Cujipers P et al, The efficacy of psychotherapy and pharmacotherapy in treating depressive and anxiety disorders: a meta‐analysis of direct comparisons, World Psychiatry. 2013, PMC3683266. "...In OCD, the outcomes are rather straightforward in that psychotherapy is clearly more efficacious than antidepressants, even adjusting for quality and other characteristics of the studies. ..."
[6] Hu et al, Incidence and duration of side effects and those rated as bothersome with selective serotonin reuptake inhibitor treatment for depression: patient report versus physician estimate, J Clin Psychiatry. 2004, PMID: 15291685
[7] Carvalho AF et al, The Safety, Tolerability and Risks Associated with the Use of Newer Generation Antidepressant Drugs: A Critical Review of the Literature, Psychother Psychosom. 2016, https://goo.gl/wiPzR9.
[8] Nat’l Institute of Health, Antidepressant Medications for Children and Adolescents: Information for Parents and Caregivers, copied 1/5/17 https://goo.gl/nicPm8.
[9] Sharma T et al, Suicidality and aggression during antidepressant treatment: systematic review and meta-analyses based on clinical study reports, BMJ. 2016, PMCID: PMC4729837.
[10] Vittengl JR, Poorer Long-Term Outcomes among Persons with Major Depressive Disorder Treated with Medication, Psychother Psychosom. 2017, PMID: 28903116. Hengartner MP et al, Antidepressant Use Prospectively Relates to a Poorer Long-Term Outcome of Depression: Results from a Prospective Community Cohort Study over 30 Years, Psychother Psychosom. 2018, PMID: 29680831.
[11] CNN Interview, How antidepressant withdrawal 'can trap people', Amanpour, 2018, https://goo.gl/cdLrdY.
[12] Read J et al, Adverse emotional and interpersonal effects reported by 1829 New Zealanders while taking antidepressants, Psychiatry Res. 2014, PMID: 24534123, Davies J et al, A systematic review into the incidence, severity and duration of antidepressant withdrawal effects: Are guidelines evidence-based?, Addictive Behaviors, 2018, https://goo.gl/8BbdgZ. [Note: 56% Prevalence * 46% severity prevalence within withdrawl group = 25.76% overall severity prevalence]
[13] Renoir T, Selective serotonin reuptake inhibitor antidepressant treatment discontinuation syndrome: a review of the clinical evidence and the possible mechanisms involved, Front. Pharmacol, 2013, PMCID: PMC3627130. Wilson E et al, A review of the management of antidepressant discontinuation symptoms, Ther Adv Psychopharmacol. 2015, PMCID: PMC4722507.
[14] Stockmann T et al, SSRI and SNRI withdrawal symptoms reported on an internet forum, Int J Risk Saf Med. 2018, PMID:29758951.
[15] Bala A et al, Post-SSRI Sexual Dysfunction: A Literature Review, Sexual Medicine Reviews, 2018, PMID: 28778697.
[16] Rütgen, M, Antidepressant treatment, not depression, leads to reductions in behavioral and neural responses to pain empathy, Translational Psychiatry, 2019. https://go.nature.com/2T0tHlu.
[17] Paddock C, The FDA approve esketamine nasal spray for severe depression, Medical News Today, 2019, http://bit.ly/35Oxx7D.
[18] Lacasse J et al, Serotonin and Depression: A Disconnect between the Advertisements and the Scientific Literature, PLOS Medicine, 2005, https://goo.gl/q2oIQa; Cowen P et al, What has serotonin to do with depression?, World Psychiatry. 2015, PMCID: PMC4471964. Laughren T, Treating Depression: Is there a placebo effect?, CBS News, 60 Minutes broadcast, 2012, https://goo.gl/ug78Av. ["The experts in the field now believe that that theory is a gross oversimplification"]; Belmaker R et al, Major Depressive Disorder, NEJ Med, 2008,,PMID: 18172175. ["Numerous studies of norepinephrine and serotonin metabolites in plasma, urine, and cerebrospinal fluid, as well as postmortem studies of the brains of patients with depression, have yet to identify the purported deficiency reliably."]
[19] Ashton H, Guidelines for the rational use of benzodiazepines. When and what to use, Drugs 1994, PMID: 7525193. “… As hypnotics, benzodiazepines are mainly indicated for transient or short term insomnia, for which prescriptions should if possible be limited to a few days, occasional or intermittent use, or courses not exceeding 2 weeks…Diazepam is usually the drug of choice, given in single doses, very short (1 to 7 days) or short (2 to 4 weeks) courses, and only rarely for longer term treatment.”
[20] Perlis RH et al, Benzodiazepine use and risk of recurrence in bipolar disorder: a STEP-BD report, J Clin Psychiatry. 2010, PMID: 20193647. “…After adjusting for potential confounding variables, the hazard ratio for mood episode recurrence among benzodiazepine-treated patients was 1.21 (95% CI, 1.01-1.45).… Benzodiazepine use may be associated with greater risk for recurrence of a mood episode among patients with bipolar I and II disorder…” Dodds TJ, Prescribed Benzodiazepines and Suicide Risk: A Review of the Literature, Prim Care Companion CNS Disord. 2017, PMID: 28257172. Note: “…The majority of studies found that benzodiazepines were associated with increased suicide risk. This finding was consistent across various populations and different types of research…”; Gale C, Anxiety Disorder, BMJ 2000, PMC1118960.
[21] FDA, FDA requires strong warnings for opioid analgesics, prescription opioid cough products, and benzodiazepine labeling related to serious risks and death from combined use, 2016, https://goo.gl/cRk3pk.
[22]. FDA, FDA Requiring Labeling Changes for Benzodiazepines, News Release, 2020, https://bit.ly/3hYTVzW.
[23] American Addiction Centes, How Long Do Benzo Withdrawal Symptoms Last?, 2018, copied November 2018 from https://goo.gl/rF6PP9, "...BENZODIAZEPINES ARE NOT INTENDED TO BE TAKEN LONG-TERM, AS PROLONGED USE OR ABUSE CAN CAUSE THE BRAIN TO BECOME BOTH PHYSICALLY AND PSYCHOLOGICALLY DEPENDENT ON THEM."
[24] Lembke, A et al, Our Other Prescription Drug Problem, New England Journal of Medicine, 2018, PMID: 2946616, https://goo.gl/vwAbhb.
[25] Dell’osso B et al, Do benzodiazepines still deserve a major role in the treatment of psychiatric disorders? A critical reappraisal. Eur Psychiatry. 2013 ,PMID: 22521806 ; Salzman C, The benzodiazepine controversy: therapeutic effects versus dependence, withdrawal, and toxicity, Harv Rev Psychiatry.1997 PMID: 9385004, “…Controversy has swirled around the use of benzodiazepines since their introduction, and show no signs of abating."
[26] Olfson M, King M, Schoenbaum M. Benzodiazepine use in the United States. JAMA Psychiatry. 2015, PMID: 25517224.
[27] Wagner C, Choices in Recovery, Onward Mental Health Press, 2019, https://goo.gl/jW6kHU.
[28] McHugh et al, Patient preference for psychological vs. pharmacological treatment of psychiatric disorders: a meta-analytic review, 2013, Journal of Clinical Psychiatry, PMC4156137.
[29] Gupta S, A Prescription for "Deprescribing" in Psychiatry, Psychiatr Serv. 2016 PMID: 26975524. Ontario Pharmacy Evidence Network, Deprescribing Guidelines, https://goo.gl/8VpYFx. Grudnikoff E et al, Deprescribing in Child and Adolescent Psychiatry—A Sorely Needed Intervention, Am J Therapeutics, 2017, PMID: 28059976. Gupta, S et al, Deprescribing antipsychotic medications in psychotic disorders: How and why? Betham Science, 2018, https://goo.gl/mR9jJ1; Reeve E et al, Review of deprescribing processes and development of an evidence-based, patient-centred deprescribing process, Br J Clin Pharmacol. 2014, PMCID: PMC4239968.
[30] Duckworth K, The Sensible Use of Psychiatric Medications, NAMI Advocate Magazine, Winter 2013, https://goo.gl/GMIuSU.
[31] Mental Health America, Complementary & Alternative Medicine for Mental Health, 2013, http://goo.gl/fTQlAo.
[32] The American Psychiatric Association has formed the “APA Caucus on Complementary, Alternative and Integrative Medicine”, http://bit.ly/2OXtXSj.
[33] James Scully (MD, APA Medical Director and CEO), excerpt from a video of him speaking to the APA’s participation in the Choosing Wisely® campaign, 2013, http://goo.gl/TrEZdx, copied 2015.
[34] Hall H et al, Nurses’ communication regarding patients’ use of complementary and alternative medicine, ScienceDirect, 2018, https://goo.gl/LNUkrX.
[35] Martins C et al, Quaternary prevention: reviewing the concept Quaternary prevention aims to protect patients from medical harm, Eur J Gen Pract, 2018, PMC5795741; European Union of General Practitioners/Family Physicians, UEMO position on Disease Mongering / Quaternary Prevention, 2011, https://goo.gl/usrpEC. “Preventive”, “restorative”, “symptom relief” and “over-care avoidance” are more descriptive terms and used in place of “primary”, “secondary”, “tertiary” and “quaternary” used in these references.