share
Bipolar

Psychiatric Drug Therapy
Five categories of drugs are commonly used to treat the mania and depression of bipolar. Research supports that they can reduce symptoms and the frequency of relapse. Regrettably, they are far from a complete solution.
Bipolar is best viewed in a broader context that considers drugs' partial effectiveness, risks, and limitations as well as the many evidence-based nondrug options available (see free monograph). This full view helps individuals and their practitioners make the most informed choices about care.
Bipolar drugs benefits, risks, & limitations
A sobering review of gold standard evidence
The most common treatment for bipolar is a combination of psychiatric drugs (called polypharmacy) that may include antipsychotics, prescription lithium (lithium carbonate), anticonvulsants, antidepressants, and benzodiazepines.
One study found that 72% of bipolar patients were taking 2 or more drugs, 55% were on 3 or more, and 36% were on 4 or more. It isn't unusual for people with bipolar to take as many as 6 different drugs. [1]
A big picture view of bipolar drugs.
Bipolar drugs have been well-studied in hundreds of gold standard trials (see infographic). Many studies show that bipolar drugs work - they generally produce better symptom relief than placebo (sugar pills). But to make informed trade-off decisions on bipolar care, we must consider the odds they'll work. Regrettably, those odds are modest - about 1 in 5.
Consider lithium for mania. Many bipolar studies show us that we have a 31% chance of substantial mania relief in 1-2 months without using drugs. [2] For reasons we don’t fully understand, our natural healing ability - the placebo effect - works. If you want to boost your odds by 16%, you can take lithium. [3] You will then have a 47% chance of substantial mania relief in 1-2 months (31% attributable to the placebo effect and 16% attributable to lithium).
For bipolar depression, the placebo effect is even more powerful. 39% of people see substantial improvement in 1-2 months without drugs. Taking an antipsychotic (lurasidone) boosts your odds to 59% (39% attributable to the placebo effect and 20% attributable to lurasidone).
Surprisingly, our natural healing ability is twice as powerful as our best gold standard drugs - 1.9X for mania (31%/16%) and 1.95X for depression (39%/20%).
The limited effectiveness of bipolar drugs comes with near-universal side effects: 86% of people who take antidepressants experience them [4] and 94% of people who take antipsychotics.[5] Side effects include chronic kidney disease with lithium, tremors, nausea, cognitive decline, sedation, sizable weight gain, sexual dysfunction, addiction (with benzodiazepines) and withdrawal difficulties. The infographic gives a sense of some of the major side effects for each of the five bipolar drug classes.
The considerable evidence against antidepressants.
The largest-ever federally funded trial for bipolar depression found that antidepressants don't work (don't outperform sugar pills) when added to mood stabilizers. [6] And most people taking bipolar drugs are on mood stabilizers. [7] Gold-standard meta-analyses and systematic reviews in 2001, 2008, 2011, 2012, 2013, 2014, and 2016 all reached variations of the same conclusion: antidepressants don't work for bipolar. [8] One meta-analysis concluded: "Existing evidence of efficacy does not support the short-term or long-term application of antidepressant therapy in patients with bipolar." [9] Another warns that the research "suggests an unfavorable risk / benefit relationship for long-term antidepressant treatment in bipolar disorder". [10]
This scientific reality collides with a prescribing reality: 30-81% of people treated for bipolar depression are taking antidepressants. This disconnect is the largest controversy in bipolar care. [11]
To attempt to resolve it, an expert global task force was convened in 2013. They found insufficient evidence to make any broad statements supporting antidepressants. [12] Bottom line: antidepressant prescribing for bipolar depression is very common, but expert consensus and extensive research don't support the practice.
A variety of contributing factors influence this situation:
-
Country prescribing guidelines are inconsistent. Some advocate antidepressants beyond the evidence and expert consensus.
-
Many people were started on antidepressants before the weakness of the underlying research was fully understood.
-
Antidepressant withdrawal symptoms, a reality for over half the people who take them, often make it hard to get off antidepressants once started. [13]
Although stand-alone antidepressants are generally considered a poor choice, the debate has turned to add-on use.One add-on antidepressant is FDA approved when combined with one antipsychotic, since it has shown to have depressive benefit. Unfortunately, this combination is almost as likely to harm (primarily substantial weight gain and metabolic issues) as it is to help.
Drugs are not the savior nor the enemy.
Although drugs are by far the most common solution, they rarely deliver recovery by themselves. Some people find them crucial to their independence. Others find them intolerable. The good news is that there is a new paradigm in mental health that offers many additional evidence-based options.
A New Paradigm: Integrative Mental Health
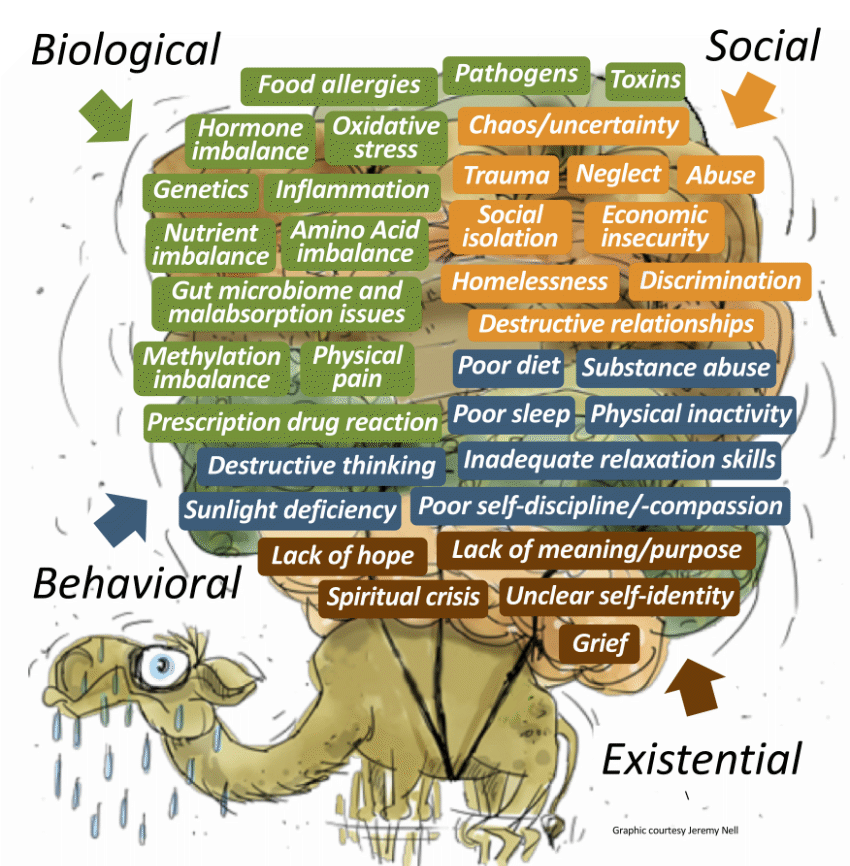
Looking beyond symptoms to causes. Many practitioners are adopting a new paradigm that looks beyond drugs. They see numerous factors dynamically interacting to cause mental distress - many we understand, others we don't. The combined weight of these factors can lead to episodes of mania or depression, and sometimes "break the camel's back" and precipitate major bipolar crisis (see graphic).
Offering individualized care. Integrative practitioners delve deeply into the unique constellation of causative factors facing each individual using detailed diagnostic tools. From this analysis they create personalized treatment plans.
Using a broad menu of options. Integrative Mental Health treatment plans nearly always include targeted evidence-based nondrug options. These options are drawn from 27 broad nondrug approaches shown effective for mental wellness. Nearly all options can be used with drugs, they typically have far fewer and milder side effects than drugs, and in many cases their use can reduce - and in some cases eliminate - the need for drugs.
Delivering better outcomes. Conventional psychiatry focuses on symptoms and brain chemistry and is drug-centric. Integrative Mental Health reasserts the importance of causes and the human experience. Limiting yourself to drugs limits your avenues to wellness and avoids the symptom improvement available in nondrug options.
Defining a new discipline. Many psychiatrists, GPs, nurse practitioners, naturopaths, therapists, medical specialists, and others are joining the paradigm shift to Integrative Mental Health, spanning the best of drug and non-drug care. These practitioners see that our mind, body, and emotions require a more holistic solution than pills alone can provide. They acknowledge a role for drugs, but consider them with great caution, especially for the developing personhood of children.

Wellness Continuum
4 categories of bipolar care

Adapted from the U.S. Institute of Medicine and European Union of General Practitioners/Family Physicians. [26]
Preventive
Preventive approaches help avoid symptoms. These include proper diet, aerobic exercise, mindfulness, stress management, ensuring gut-health, sleep hygiene, social interaction, bright natural light, mind-body disciplines (especially yoga) and more.
Restorative
Two methods work to address causative factors of bipolar.
Biomedical practitioners (see practitioner finder) seek to understand your unique bio-individuality using robust lab tests. 25% of the time mental distress is caused or influenced by physical issues. Testing helps uncover nutrient imbalances, hormonal issues, amino acid irregularities, food allergies, inflammation, and other issues directly associated with bipolar symptoms. Treatment is then targeted at specific issues identified.
Using nutrient therapy, 75% of people with bipolar report significant symptom improvement and the ability to reduce medication, while about 5% can eliminate medication altogether. See this short video from Dr. William Walsh, PhD, a leader in nutrient therapy.
Psychosocial practitioners help address painful experience including trauma, dysfunctional relationships, unhelpful thinking, and more. Cognitive Behavioral Therapy is proven effective in improving bipolar mania, depression, and avoiding relapse, while improving functioning. Peer support from those who live in recovery offers a valuable "been there" perspective. Spiritually-sensitive care helps those experiencing difficult personal growth.
Symptom Relief
Symptom relief addresses symptoms not removed by preventive and restorative care. Select herbs, nutrients, sensory therapies, probiotics, and gentle electrical stimulation have been shown effective.
Over-care
Avoidance
Over-care avoidance limits interventions (usually drugs) to only what is necessary.
Over-care can be expensive and harmful. This is especially true for those with bipolar since they often take 3-5 drugs at once. Adding a drug may reduce symptoms somewhat but comes with considerable added risk.
Unfortunately, the sheer number of individual bipolar drugs makes combination testing practically nonexistent. This creates an uncomfortable reality: although psychiatry seeks evidence-based care, it ventures beyond the evidence base for all but the simplest bipolar prescribing. As a result, significant trial-and-error is often needed when using bipolar drugs.
Studies show that the greater the number of drugs taken, the greater the suicide risk and the worse the outcomes. [18] Most risky is taking two or more antipsychotics. The more antipsychotics taken simultaneously, the shorter the life span. [19]
Many psychiatrists are considering de-prescribing plans for their patients given the troubling risk/benefit profile of being on a cocktail of drugs. [20]
Your life. Your choice.
The limited effectiveness and many challenges of the five classes of bipolar drugs make their risk/reward profile much less favorable than most people think.
This is one reason why key voices in mainstream psychiatry support nondrug options.
-
NAMI. Dr. Kenneth Duckworth, Medical Director of the National Alliance on Mental Illness, is clear: "... psychiatric medications... are rarely enough to promote recovery alone... Use of non-medication strategies is crucial for most clinical situations." [21]
-
Mental Health America advocates many nondrug options. [22]
-
American Psychiatric Association sponsors a special interest caucus of psychiatrists grounded in Integrative Mental Health. [23]
In addition, Dr. James Scully, past American Psychiatric Association Medical Director and CEO, understands well the implications of psychiatric drugs. He says:
Physicians and patients together should be thinking carefully, ‘Are the medications really needed and are there downsides and negative consequences for overuse?’... Patients really need to be a part of the decision… of their own treatments. [24]
Carefully consider Dr. Scully’s question – your recovery may well depend on it – and be an active participant in determining your treatment. If you make adjustments to the drugs you take, do so slowly under practitioner care.
Doctors and patients alike want the transparent sharing of the pros and cons of all treatment options. However, this communication is often inadequate. Studies note that information on the risks, side effects, and withdrawal difficulties of drugs is often poor. In addition, communication about nondrug options rarely occurs. [25]
Always work closely with your doctors as you make care decisions. They are your trusted guides. Also independently educate yourself since Integrative Mental Health is not yet prevalent in psychiatric care. You will likely need to expand your team to include integrative practitioners if you seek to use nondrug options as part of your recovery.
Although non-drug options aren't a panacea, many people are reclaiming their lives thanks to the expanded menu of options of Integrative Mental Health. Their self-determined return to normalcy can offer you compelling and pragmatic reasons for hope.



Resources
-
Free! Bipolar Monograph - Overview of the most effective non-drug options for bipolar.
-
Choices in Recovery - Detail on evidence-based non-drug options for bipolar and other major diagnoses.
-
Understanding Bipolar - British Psychological Society.
-
Nutrient Therapy for Bipolar. William Walsh (video).
Footnote references are removed in the mobile version of this page to respect small screen sizes. They can be found in the desktop version.
share
Note: To make this material more understandable, we use commonly understood phrases to represent rigorous statistical metrics. See our definitions.
References:
[1] Weinstock LM et al, Medication burden in bipolar disorder: a chart review of patients at psychiatric hospital admission. Psychiatry Res. 2014, PMCID: PMC3968952.
[2] Sysko R et al, A systematic review of placebo response in studies of bipolar mania, J Clin Psychiatry. 2007, PMID: 17854245.
[3] Yildiz A et al, Efficacy of Antimanic Treatments: Meta-analysis of Randomized, Controlled Trials, Neuropsychopharmacology. 2011, PMC3055677.
[4] Hu et al, Incidence and duration of side effects and those rated as bothersome with selective serotonin reuptake inhibitor treatment for depression: patient report versus physician estimate, J Clin Psychiatry. 2004, PMID: 15291685
[5] Lindström E et al, Patient-rated versus clinician-rated side effects of drug treatment in schizophrenia. Clinical validation of a self-rating version of the UKU Side Effect Rating Scale (UKU-SERS-Pat), Nord J Psychiatry. 2001, PMID: 11860666. https://goo.gl/YzWtff. N
[6] National Institute of Mental Health (NIMH), Study Sheds Light on Medication Treatment Options for Bipolar Disorder, 2007, NIMH Archive, https://goo.gl/q5YGxx.
[7] Greil W et al, Pharmacotherapeutic trends in 2231 psychiatric inpatients with bipolar depression from the International AMSP Project between 1994 and 2009. J Affect Disord 2012, PMID: 22134044.
[8] Systematic reviews and meta-analyses finding no value of antidepressants over placebo.
Nemeroff CB et al, Double-blind, placebo-controlled comparison of imipramine and paroxetine in the treatment of bipolar depression, Am J Psychiatry. 2001, PMID: 11384898. https://goo.gl/z4r9ya.
National Institute of Mental Health (NIMH), Study Sheds Light on Medication Treatment Options for Bipolar Disorder, 2007, NIMH Archive, https://goo.gl/q5YGxx.
Ghaemi S et al, Long-term antidepressant treatment in bipolar disorder: meta-analyses of benefits and risks, Acta Psychiatr Scand. 2008, PMCID: PMC2718794.
Sidor MM et al, Antidepressants for the acute treatment of bipolar depression: a systematic review and meta-analysis, J Clin Psychiatry. 2011, PMID: 21034686, https://goo.gl/XtwCya,
Amit B et al, Antidepressant Treatment for Acute Bipolar Depression: An Update, Depress Res Treat. 2012, PMCID: PMC3272786;
Zhang Y et al, Antidepressants for bipolar disorder: A meta-analysis of randomized, double-blind, controlled trials, Neural Regen Res. 2013, PMCID: PMC4146170,
McInerney S et al, Review of Evidence for Use of Antidepressants in Bipolar Depression, Primary Care Companion CNS Disord. 2014, PMCID: PMC4321017.
McGirr A et al, Safety and efficacy of adjunctive second-generation antidepressant therapy with a mood stabiliser or an atypical antipsychotic in acute bipolar depression: a systematic review and meta-analysis of randomised placebo-controlled trials, Lancet Psychiatry. 2016, PMID: 28100425, https://goo.gl/TzYB1A.
[9] Zhang Y et al, Antidepressants for bipolar disorder: A meta-analysis of randomized, double-blind, controlled trials, Neural Regen Res. 2013, PMCID: PMC4146170.
[10] Ghaemi S et al, Long-term antidepressant treatment in bipolar disorder: meta-analyses of benefits and risks, Acta Psychiatr Scand. 2008, PMCID: PMC2718794.
[11] Antidepressant prescribing rates.
Greil W et al, Pharmacotherapeutic trends in 2231 psychiatric inpatients with bipolar depression from the International AMSP Project between 1994 and 2009. J Affect Disord 2012, PMID: 22134044.
Baldessarini RJ et al. Patterns of psychotropic drug prescription for U.S. patients with diagnoses of bipolar disorders. Psychiatr Serv 2007, PMID: 17215417;
Goodwin G et al, Evidence-based guidelines for treating bipolar disorder: Revised third edition recommendations from the British Association for Psychopharmacology, Journal of Psychopharmacology, 2016, PMC4922419.
[12] Pacchiarotti I et al, The International Society for Bipolar Disorders (ISBD) Task Force Report on Antidepressant Use in Bipolar Disorders, Am J Psych, 2013, PMCID: PMC4091043.
[13] Antidepressant withdrawal. Davies J et al, A systematic review into the incidence, severity and duration of antidepressant withdrawal effects: Are guidelines evidence-based?, Addictive Behaviors, 2018, https://goo.gl/8BbdgZ.
[14] Gitlin M et al, Antidepressants in bipolar depression: an enduring controversy, nt J Bipolar Disord. 2018, PMC6269438.
[15] Laughren T, Treating Depression: Is there a placebo effect?, CBS News, 60 Minutes broadcast, 2012, https://goo.gl/ug78Av.
[16] Barbui C et al, Efficacy of antidepressants and benzodiazepines in minor depression: systematic review and meta-analysis, Br J Psychiatry. 2011, PMCID: PMC3014462. Fournier JC et al, Antidepressant drug effects and depression severity: a patient-level meta-analysis. JAMA, 2010, PMCID: PMC3712503. Kirsch I et al, Initial Severity and Antidepressant Benefits: A Meta-Analysis of Data Submitted to the Food and Drug Administration, PLoS Med. 2008, PMCID: PMC2253608;
[17] Read J et al, Child Maltreatment and Psychosis: A Return to a Genuinely Integrated Bio-Psycho-Social Model. Clinical, 2008, Clinical Schizophrenia, https://goo.gl/nMLrx4.
[18] Gazalle FK et al, Polypharmacy and suicide attempts in bipolar disorder, Rev Bras Psiquiat, 2007, PMID: 17435926, https://goo.gl/4nC2S1. “...The number of suicide attempts was associated with the use of multiple drugs… ” “… There is evidence that patients who are submitted to multiple medications have an increased risk of side effects and early mortality…” . Kingsbury S, Psychopharmacology: Rational and Irrational Polypharmacy, Psychiatric Services, Aug 2001, PMID: 11474046, http://goo.gl/PFE3Rk; “… most would agree that any use of multiple medications may increase the risk of adverse effects, drug interactions, … and medication errors…”
[19] Waddington JL, Mortality in schizophrenia. Antipsychotic polypharmacy and absence of adjunctive anticholinergics over the course of a 10-year prospective study, Br J Psychiatry 1998, PMID: 9926037. Joukamaa M et al, Schizophrenia, neuroleptic medication and mortality. Br J Psychiatry, 2006, PMID: 16449697. Ito H et al, Polypharmacy and excessive dosing: psychiatrists' perceptions of antipsychotic drug prescription. Br J Psychiatry. 2005, PMID: 16135861.
[20] Gupta S, A Prescription for "Deprescribing" in Psychiatry, Psychiatr Serv. 2016 PMID: 26975524. Ontario Pharmacy Evidence Network, Deprescribing Guidelines, https://goo.gl/8VpYFx. Grudnikoff E et al, Deprescribing in Child and Adolescent Psychiatry—A Sorely Needed Intervention, Am J Therapeutics, 2017, PMID: 28059976. Gupta, S et al, Deprescribing antipsychotic medications in psychotic disorders: How and why? Betham Science, 2018, https://goo.gl/mR9jJ1; Reeve E et al, Review of deprescribing processes and development of an evidence-based, patient-centred deprescribing process, Br J Clin Pharmacol. 2014, PMCID: PMC4239968.
[21] Duckworth K, The Sensible Use of Psychiatric Medications, NAMI Advocate Magazine, Winter 2013, https://goo.gl/GMIuSU.
[22] Mental Health America, Complementary & Alternative Medicine for Mental Health, 2013, http://goo.gl/fTQlAo.
[23] The American Psychiatric Association has formed the “APA Caucus on Complementary, Alternative and Integrative Medicine”, http://bit.ly/2OXtXSj.
[24] James Scully (MD, APA Medical Director and CEO), excerpt from a video of him speaking to the APA’s participation in the Choosing Wisely® campaign, 2013, http://goo.gl/TrEZdx, copied 2015.
[25] Hall H et al, Nurses’ communication regarding patients’ use of complementary and alternative medicine, ScienceDirect, 2018, https://goo.gl/LNUkrX. ll-Party Parliamentary Group for Prescribed Drug Dependence, Antidepressant Withdrawal: a Survey of Patients’ Experience by the All-Party Parliamentary Group for Prescribed Drug Dependence, 2018, https://goo.gl/aFXv3o; All-Party Parliamentary Group for Prescribed Drug Dependence, The Patient Voice: an analysis of the personal accounts of prescribed drug dependence and withdrawal submitted to petitions in Scotland and Wales, 2018, https://goo.gl/nYEhJd.
[26] Martins C et al, Quaternary prevention: reviewing the concept Quaternary prevention aims to protect patients from medical harm, Eur J Gen Pract, 2018, PMC5795741; European Union of General Practitioners/Family Physicians, UEMO position on Disease Mongering / Quaternary Prevention, 2011, https://goo.gl/usrpEC. “Preventive”, “restorative”, “symptom relief” and “over-care avoidance” are more descriptive terms and used in place of “primary”, “secondary”, “tertiary” and “quaternary” used in these references.