share
Depression
Depression

Psychiatric Drug Therapy
Antidepressants are the most common treatment the for depression. Studies show that they can help reduce symptoms for some people with major depression. Regrettably, they are far from a complete solution.
To maximize recovery, depression is best viewed in a broader context that considers drugs' partial effectiveness, risks, and limitations as well as the many evidence-based nondrug options available (see free monograph). This full view helps individuals and their practitioners make the most informed choices about care.
Do Antidepressants Work?
Yes, but their benefit is almost entirely placebo effect
The Director of the FDA's psychiatry products confirms that conventional antidepressants work, but their benefit over placebo (sugar pills) is "rather small". [1]
This conclusion is supported by the clear evidence of many independent gold-standard drug trials. Overall, placebos eliminate 38% of depressive symptoms while conventional antidepressants alleviate 46%. [2] This 8% difference is so small that researchers note that it isn't "clinically relevant" [3] - its impact is too small to notice.
Further, these antidepressants provide no clinically noticeable benefit for minor or moderate depression [4], and their benefits are "relatively small even for severely depressed patients" [4, 5]. Only 3% of people taking antidepressants achieve a non-depressed state and stayed that way for a year. [6] Dr. James Davies gives more detail.
Ketamine (a common intravenous anesthetic) and esketamine (a patentable nasal spray variant) are drug alternatives that can rapidly reduce depression. But there are many caveats: esketamine causes significant improvement in only 14% of patients [22b], there is legitimate criticism of esketamine study quality [22c], and the drugs have unequivocal potential for serious side effects including psychosis and dissociation. [23] As a result, the FDA has placed restricted availability and tight monitoring on esketamine use. [24]
Courtesy Dr. James Davies.
Antidepressant Risks & Limitations
A sobering review of gold standard evidence
Side effects. Side effects from antidepressants are very common (see graphic): 86% of people have them, and 55% find them bothersome. [7] Side effects include gastrointestinal issues, weight gain, cardiovascular issues, Parkinsonian-like involuntary movements, and especially sexual dysfunction. [8] These may persist even after you stop using the drugs. Those on antidepressants are 50% more likely to develop Type 2 diabetes. [9] The FDA has issued their most severe black box warning for antidepressants, since they double the frequency of suicidal thoughts in those under 25. [10] Research also shows that the drugs double the likelihood of suicide and violence in adults [11] - even after discontinuing their use. [12] Antidepressants are also associated with a tripling of the frequency of aggressive behavior in children. [13]
Worse long-term outcomes. The results of multi-year antidepressant use are grim. Those on antidepressants have significantly worse depression at 9-year, 20-year, and 30-year visits compared to depressed individuals who didn't take the drugs. [14] In fact, antidepressant users are hospitalized more frequently and for over twice the duration as depressed patients who do not take the drugs. [15] Antidepressants, therefore, appear to worsen your chances of recovery.
Withdrawal difficulty. Dr. Allen Francis, noted psychiatrist and, editor of the U.S. "psychiatric bible" warns of Antidepressant Discontinuation Syndrome "It’s so easy to start an antidepressant and sometimes so very difficult to stop it." [16] Up to 63% of people experience withdrawal, almost half of those find the experience severe, usually lasting six weeks but sometimes much longer. [17, 18] Growing awareness of this problem has caused U.K guidelines to be updated to warn patients of potential severe withdrawal. [19]. 53 withdrawal symptoms have been identified including anxiety, dizziness, irritability, poor concentration, gastrointestinal problems, and insomnia. [20]
Post SSRI Sexual Dysfunction (PSSD). Evidence suggests that the sexual dysfunction common in SSRI antidepressant use may persist even after the drugs are discontinued. Common PSSD symptoms include genital anesthesia and pleasure-less or weak orgasm. There is currently no treatment for PSSD. [21]
Blunting of Empathy. Antidepressants can limit the ability to feel normal emotions. One study found that after using them for three months, people have less ability to empathize with others and scans indicate reduced activity in portions of the brain associated with empathy. [22]

Esketamine: even greater risk. The new antidepressant Esketamine comes with even greater risks than older antidepressants. FDA warnings highlights the potential for sedation, dissociation, attention and judgment problems, drug abuse, suicidal thoughts, and suicidal behavior. Two of the trials actually produced negative results. [23] As a result, the FDA has placed restricted availability and tight monitoring on the drug. [24]
Antidepressants: muted results, faulty theory
A fundamental reason for the lackluster outcomes with antidepressants is that experts now consider the underlying chemical imbalance theory of depression to be untenable and a "gross over-simplification". [25]
For many years low levels of serotonin and other brain chemicals were thought to cause depression. Serotonin-increasing antidepressants were therefore prescribed. Later, it was found that drugs that increase serotonin had the same impact as drugs that decrease it - both providing relief only slightly better than placebo. [26]
This theory was well-intended but a one-size-fits-all antidepressant approach doesn't match the complex human experience of depression. Further, a rigorous study of possible genetic causes for depression came up empty. [27] Many psychiatrists and researchers agree that a more sophisticated theory and more robust therapeutic approach is needed. Dr. Joanna Moncrieff explains in this video.
Courtesy Dr. Joanna Moncrieff.
A New Paradigm: Integrative Mental Health
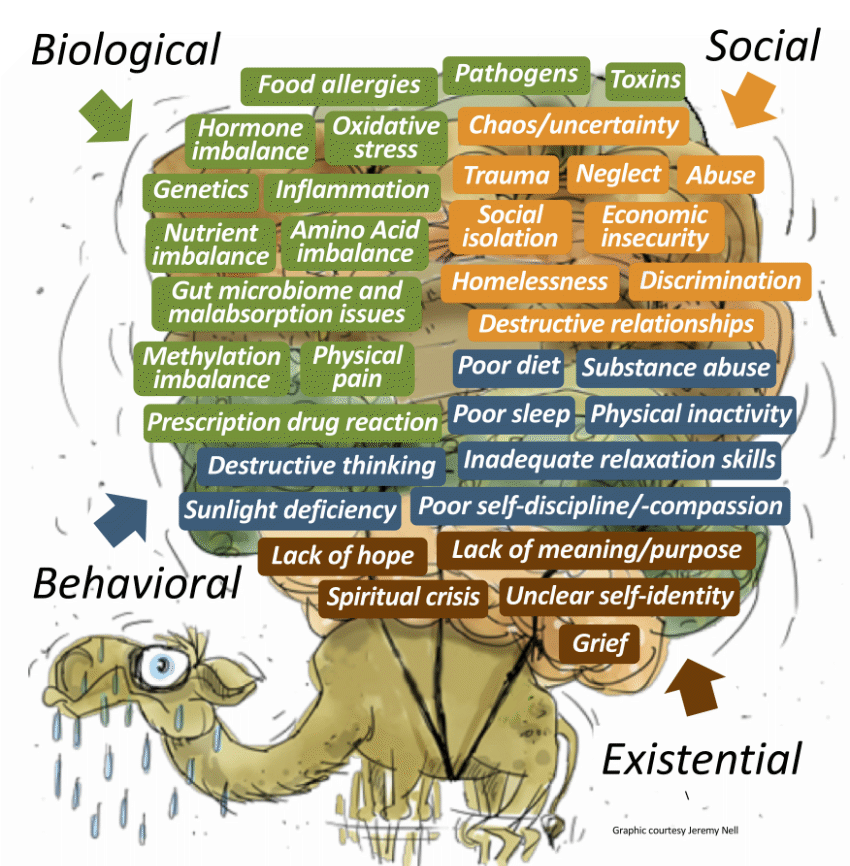
Looking beyond symptoms to causes. Many practitioners are adopting an extended paradigm that looks beyond drugs. They see numerous factors dynamically interacting to cause mental distress - many we understand, others we don't. The combined weight of these factors can lead to episodes of depression and sometimes "break the camel's back" and precipitate major depressive crisis (see graphic).
Offering personalized care. Integrative practitioners delve deeply into the unique constellation of causative factors facing each individual using detailed diagnostic tools. From this analysis they create personalized treatment plans.
Using a broad menu of options. Integrative Mental Health treatment plans nearly always include targeted evidence-based nondrug options. These options are drawn from 27 broad nondrug approaches shown effective for mental wellness. [28] Nearly all options can be used with drugs, they typically have far fewer and milder side effects than drugs, and in many cases their use can reduce - and in some cases eliminate - the need for drugs.
Delivering better outcomes. Drugs alone rarely deliver recovery. Thankfully, you have options. Although much less studied than drugs, there are hundreds of gold-standard trials that show depressive symptom relief from a wide variety of nondrug options. Limiting yourself to drugs limits your avenues to wellness.
Providing options people prefer. A review of 34 studies found that people prefer psychological treatments over drugs 3 to 1. [29]
Defining a new discipline. Many psychiatrists, GPs, nurse practitioners, naturopaths, therapists, medical specialists, and others are joining the paradigm shift to Integrative Mental Health, embracing the best of drug and non-drug care. These practitioners see that our mind, body, and emotions require a more holistic solution than pills alone can provide. They acknowledge a role for drugs, but consider them with great caution, especially for the developing brain and personhood of children.

Wellness Continuum
4 forms of care for
depression

Adapted from the U.S. Institute of Medicine and European Union of General Practitioners/Family Physicians. [41]
Back to Basics
Preventive
Preventive approaches help us avoid depression. These include proper diet, aerobic exercise, mindfulness, stress management, social interaction, optimizing gut health, being in bright natural light, mind-body disciplines (especially yoga) and more.
Restorative
Two methods work to address causative factors of depression.
Biomedical practitioners (see practitioner finder) help identify and support your unique bio-individuality using robust lab tests. 25% of the time mental distress is caused or influenced by physical issues. [30] Testing helps uncover nutrient imbalances, hormonal issues, amino acid irregularities, food allergies, inflammation, and other issues that are directly associated with depression. Treatment is grounded in individualized nutrient therapy.
Psychosocial practitioners help address painful human experience including trauma, dysfunctional relationships, unhelpful thinking, and more. Cognitive Behavioral Therapy works as well as antidepressants for depression with lower side effects and relapse rates, and it has sustained long-term benefits, unlike antidepressants. [31] Peer support from those who live in recovery offers a valuable "been there" perspective. Spiritually-sensitive care can help those experiencing difficult personal growth.
Symptom Relief
Symptom relief addresses residual symptoms not removed by preventive and restorative care. Various herbs, nutrients, sensory therapies and gentle electrical stimulation have been shown effective.
Over-care
Avoidance
Over-care avoidance limits interventions to only what is necessary. Too much care can be expensive and harmful. The research says:
Antidepressants don't work well. They provide little or no benefit for mild/moderate depression and only slight benefit for severe cases. They also can stimulate bipolar mania.
Stopping antidepressant use can be hard. Many people have withdrawal symptoms that mimic the original depressive symptoms.
Electroconvulsive therapy (ECT) can cause brain damage and is poorly supported by research. [32]
You have other good options. Read our monograph for an overview.
Psychiatrists are considering de-prescribing plans for their patients based on antidepressant's risk/benefit profile. [33]
Your life. Your choice.
Although antidepressants provide benefit for some people, their limited effectiveness and many downsides make their risk/reward profile much less favorable than most people think. In fact, researchers who have examined the breadth of drug studies assert that "the potential small beneficial effects [of antidepressants] seem to be outweighed by harmful effects." [34].
This is one reason why key voices in mainstream psychiatry support nondrug options.
-
NAMI. Dr. Kenneth Duckworth, Medical Director of the National Alliance on Mental Illness, is clear: "... psychiatric medications... are rarely enough to promote recovery alone... Use of non-medication strategies is crucial for most clinical situations." [35]
-
Mental Health America advocates many nondrug options. [36]
-
American Psychiatric Association sponsors a special interest caucus of psychiatrists grounded in Integrative Mental Health. [37]
In addition, Dr. James Scully, past American Psychiatric Association Medical Director and CEO, understands well the implications of psychiatric drugs. He says:
Physicians and patients together should be thinking carefully, ‘Are the medications really needed and are there downsides and negative consequences for overuse?’... Patients really need to be a part of the decision… of their own treatments. [38]
Carefully consider Dr. Scully’s question – your recovery may well depend on it – and be an active participant in determining your treatment. If you make adjustments to the drugs you take, do so slowly under practitioner care.
Doctors and patients alike want the transparent sharing of the pros and cons of all treatment options. However, this communication is often inadequate. Studies note that people rarely receive adequate information from their doctors on the withdrawal difficulties, risks, and side effects of antidepressants. [39] In addition, communication about nondrug options rarely occurs. [40]
Always work closely with your doctors as you make care decisions. They are your trusted guides. At the same time, independently educate yourself on nondrug options since Integrative Mental Health is not yet prevalent in psychiatric care. You will likely need to expand your team to include integrative practioners if you seek to use nondrug options as part of your recovery.
Although non-drug options aren't a panacea and access can be a challenge, many people are reclaiming their lives thanks to the expanded menu of options of Integrative Mental Health. Their self-determined return to normalcy can offer you compelling and pragmatic reasons for hope.



Resources
-
Free! Depression Monograph - Overview of non-drug options
-
Choices in Recovery - Detail on evidence-based non-drug options for depression and other major diagnoses.
-
American Psychiatric Associations report on nondrug therapies for depression.
Footnote references are removed in the mobile version of this page to respect small screen sizes. They can be found in the desktop version.
share
Note: To make this material more understandable, we use commonly understood phrases to represent rigorous statistical metrics. See our definitions.
References:
[1] Laughren T, Treating Depression: Is there a placebo effect?, CBS News, 60 Minutes broadcast, 2012, https://goo.gl/ug78Av.
[2] Khan, A et al, Antidepressants versus placebo in major depression: an overview. World Psychiatry, 2015, PMCID: PMC4592645.
[3] Kirsch I et al, The emperor's new drugs: an analysis of antidepressant medication data submitted to the U.S. Food and Drug Administration. Prev Treat. 2002, https://goo.gl/YtAL6J.
[4] Barbui C et al, Efficacy of antidepressants and benzodiazepines in minor depression: systematic review and meta-analysis, Br J Psychiatry. 2011, PMCID: PMC3014462. Fournier JC et al, Antidepressant drug effects and depression severity: a patient-level meta-analysis. JAMA, 2010, PMCID: PMC3712503.
[5] Kirsch I et al, Initial Severity and Antidepressant Benefits: A Meta-Analysis of Data Submitted to the Food and Drug Administration, PLoS Med. 2008, PMCID: PMC2253608;
[6] Pigott HE et al, Efficacy and Effectiveness of Antidepressants: Current Status of Research, Psychother Psychosom 2010, PMID: 20616621.
[7] Hu et al, Incidence and duration of side effects and those rated as bothersome with selective serotonin reuptake inhibitor treatment for depression: patient report versus physician estimate, J Clin Psychiatry. 2004, PMID: 15291685
[8] Carvalho AF et al, The Safety, Tolerability and Risks Associated with the Use of Newer Generation Antidepressant Drugs: A Critical Review of the Literature, Psychother Psychosom. 2016, https://goo.gl/wiPzR9.
[9] Salvi V, The risk of new-onset diabetes in antidepressant users – A systematic review and meta-analysis, PLoS One. 2017, PMCID: PMC5536271.
[10] Nat’l Institute of Health, Antidepressant Medications for Children and Adolescents: Information for Parents and Caregivers, copied 1/5/17 https://goo.gl/nicPm8.
[11] Bielefeldt AØ et al, Precursors to suicidality and violence on antidepressants: systematic review of trials in adult healthy volunteersJ R Soc Med. 2016, PMC5066537; Hengartner M, Newer-Generation Antidepressants and Suicide Risk in Randomized Controlled Trials: A Re-Analysis of the FDA Database. Psychotherapy and Psychosomatics, 2019, http://bit.ly/2KH8Fop.
[12] Lagerberg T et al,. Associations between selective serotonin reuptake inhibitors and violent crime in adolescents, young, and older adults – A Swedish register-based study, 2020, In press, European Neuropsychopharmacology., https://bit.ly/37AQuf2.
[13] Sharma T et al, Suicidality and aggression during antidepressant treatment: systematic review and meta-analyses based on clinical study reports, BMJ. 2016, PMCID: PMC4729837.
[14] Vittengl JR, Poorer Long-Term Outcomes among Persons with Major Depressive Disorder Treated with Medication, Psychother Psychosom. 2017, PMID: 28903116. Hengartner MP et al, Antidepressant Use Prospectively Relates to a Poorer Long-Term Outcome of Depression: Results from a Prospective Community Cohort Study over 30 Years, Psychother Psychosom. 2018, PMID: 29680831.
[15] Hengartner M.P et al, Antidepressant Use During Acute Inpatient Care Is Associated With an Increased Risk of Psychiatric Rehospitalisation Over a 12-Month Follow-Up After Discharge. 2019, Frontiers in Psychiatry, PMC6396716.
[16] CNN Interview, How antidepressant withdrawal 'can trap people', Amanpour, 2018, https://goo.gl/cdLrdY.
[17] Read J et al, Adverse emotional and interpersonal effects reported by 1829 New Zealanders while taking antidepressants, Psychiatry Res. 2014, PMID: 24534123, Davies J et al, A systematic review into the incidence, severity and duration of antidepressant withdrawal effects: Are guidelines evidence-based?, Addictive Behaviors, 2018, https://goo.gl/8BbdgZ. [Note: 56% Prevalence * 46% severity prevalence within withdrawl group = 25.76% overall severity prevalence]
[18] Royal College of Psychiatrists (2012) Coming off antidepressants. Website www.rcpsych. ac.uk/healthadvice/treatmentswellbeing/antidepressants/comingoffantidepressants. aspx. (Accessed Feb 2018)
[19] National Institute for Care and Health Excellence (NICE). Depression in adults: recognition and management. 2019, http://bit.ly/2J9Ioiv.
[20] Renoir T, Selective serotonin reuptake inhibitor antidepressant treatment discontinuation syndrome: a review of the clinical evidence and the possible mechanisms involved, Front. Pharmacol, 2013, PMCID: PMC3627130. Wilson E et al, A review of the management of antidepressant discontinuation symptoms, Ther Adv Psychopharmacol. 2015, PMCID: PMC4722507.
[21] Bala A et al, Post-SSRI Sexual Dysfunction: A Literature Review, Sexual Medicine Reviews, 2018, PMID: 28778697.
[22] Rütgen, M, Antidepressant treatment, not depression, leads to reductions in behavioral and neural responses to pain empathy, Translational Psychiatry, 2019. https://go.nature.com/2T0tHlu.
[22b] Citrom L et al, Appraising esketamine nasal spray for the management of treatment-resistant depression in adults: Number needed to treat, number needed to harm, and likelihood to be helped or harmed, J Affect Disord 2020, PMID: 32479321.Note: Esketamine Number Needed to Treat is in the range of 6-8. 14% represents the middle of the range (1/7).
[22c] McIntyre RS et al, Synthesizing the Evidence for Ketamine and Esketamine in Treatment-Resistant Depression: An International Expert Opinion on the Available Evidence and Implementation, ajp.psychiatryonline.org, 2020, https://bit.ly/3C79eRD.
[23] Gastaldon C et al: Post-marketing safety concerns with esketamine: a disproportionality analysis of spon- taneous reports submitted to the FDA Adverse Event Reporting System. Psychother Psychosom 20210, Are we repeating mistakes of the past? A review of the evidence for esketamine. The British Journal of Psychiatry. Published online by Cambridge University Press, 2020, https://bit.ly/3hqhum6.
[24] Paddock C, The FDA approve esketamine nasal spray for severe depression, Medical News Today, 2019, http://bit.ly/35Oxx7D.
[25] Lacasse J et al, Serotonin and Depression: A Disconnect between the Advertisements and the Scientific Literature, PLOS Medicine, 2005, https://goo.gl/q2oIQa; Cowen P et al, What has serotonin to do with depression?, World Psychiatry 2015, PMCID: PMC4471964. Laughren T, Treating Depression: Is there a placebo effect?, CBS News, 60 Minutes broadcast, 2012, https://goo.gl/ug78Av. ["The experts in the field now believe that that theory is a gross oversimplification"]; Belmaker R et al, Major Depressive Disorder, NEJ Med, 2008,,PMID: 18172175. ["Numerous studies of norepinephrine and serotonin metabolites in plasma, urine, and cerebrospinal fluid, as well as postmortem studies of the brains of patients with depression, have yet to identify the purported deficiency reliably."]
[26] Wagstaff AJ, Tianeptine: a review of its use in depressive disorders, CNS Drugs. 2001, PMID: 11463130, https://goo.gl/brq2r7.
[27] Border R et al, No Support for Historical Candidate Gene or Candidate Gene-by-Interaction Hypotheses for Major Depression Across Multiple Large Samples. 2009, American Journal of Psychiatry.
[28] Wagner C, Choices in Recovery, Onward Mental Health Press, 2019, https://goo.gl/jW6kHU.
[29] McHugh et al, Patient preference for psychological vs. pharmacological treatment of psychiatric disorders: a meta-analytic review, 2013, Journal of Clinical Psychiatry, PMC4156137.
[30] Koranyi EK et al, Physical illnesses underlying psychiatric symptoms, Psycho Psychosom. 1992, PMID: 1488499, http://goo.gl/V9Wi23.; Koran L, MEDICAL EVALUATION FIELD MANUAL, 1991, http://goo.gl/TPNL9t, copied 10/30/2013.; Hall RC, Physical illness manifesting as psychiatric disease. II. Analysis of a state hospital inpatient population, Arch Gen Psychiatry. 1980, PMID: 7416911.
[31] Cujipers P et al, Psychological treatments are as effective as pharmacotherapies in the treatment of adult depression: a summary from Randomized Clinical Trials and neuroscience evidence, https://goo.gl/C67zXw.; Vaswani A, Non-Pharmacological Treatments (NPTs) for Depression Are Effective, Mad in America, https://goo.gl/Zrlvjh; Khan, A et al, Antidepressants versus placebo in major depression an overview. World Psychiatry (Figure 1, Blinded studies), 2015, PMCID: PMC4592645; Farah WH et al, Non-pharmacological treatment of depression: a systematic review and evidence map, Evid Based Med. 2016, PMID: 27836921.
[32] Read J et al, Electroconvulsive therapy for depression: A review of the quality of ECT versus sham ECT trials and meta-analyses. Ethical Human Psychology and Psychiatry, 2020, https://bit.ly/3cJnEKH.
[33] Gupta S, A Prescription for "Deprescribing" in Psychiatry, Psychiatr Serv. 2016 PMID: 26975524. Ontario Pharmacy Evidence Network, Deprescribing Guidelines, https://goo.gl/8VpYFx. Grudnikoff E et al, Deprescribing in Child and Adolescent Psychiatry—A Sorely Needed Intervention, Am J Therapeutics, 2017, PMID: 28059976. Gupta, S et al, Deprescribing antipsychotic medications in psychotic disorders: How and why? Betham Science, 2018, https://goo.gl/mR9jJ1; Reeve E et al, Review of deprescribing processes and development of an evidence-based, patient-centred deprescribing process, Br J Clin Pharmacol. 2014, PMCID: PMC4239968.
[34] Jakobsen, JC et al, Selective serotonin reuptake inhibitors versus placebo in patients with major depressive disorder. A systematic review with meta-analysis and Trial Sequential Analysis,2017, BMC Psych, https://goo.gl/FF9lqo.
[35] Duckworth K, The Sensible Use of Psychiatric Medications, NAMI Advocate Magazine, Winter 2013, https://goo.gl/GMIuSU.
[36] Mental Health America, Complementary & Alternative Medicine for Mental Health, 2013, http://goo.gl/fTQlAo.
[37] The American Psychiatric Association has formed the “APA Caucus on Complementary, Alternative and Integrative Medicine”, http://bit.ly/2OXtXSj.
[38] James Scully (MD, APA Medical Director and CEO), excerpt from a video of him speaking to the APA’s participation in the Choosing Wisely® campaign, 2013, http://goo.gl/TrEZdx, copied 2015.
[39] All-Party Parliamentary Group for Prescribed Drug Dependence, Antidepressant Withdrawal: a Survey of Patients’ Experience by the All-Party Parliamentary Group for Prescribed Drug Dependence, 2018, https://goo.gl/aFXv3o; All-Party Parliamentary Group for Prescribed Drug Dependence, The Patient Voice: an analysis of the personal accounts of prescribed drug dependence and withdrawal submitted to petitions in Scotland and Wales, 2018, https://goo.gl/nYEhJd.
[40] Hall H et al, Nurses’ communication regarding patients’ use of complementary and alternative medicine, ScienceDirect, 2018, https://goo.gl/LNUkrX.
[41] Martins C et al, Quaternary prevention: reviewing the concept Quaternary prevention aims to protect patients from medical harm, Eur J Gen Pract, 2018, PMC5795741; European Union of General Practitioners/Family Physicians, UEMO position on Disease Mongering / Quaternary Prevention, 2011, https://goo.gl/usrpEC. “Preventive”, “restorative”, “symptom relief” and “over-care avoidance” are more descriptive terms and used in place of “primary”, “secondary”, “tertiary” and “quaternary” used in these references.